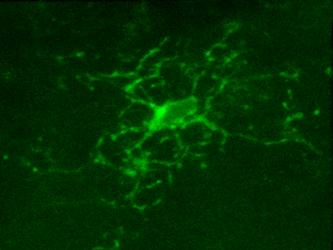
 Microglia, resident immune cells of the brain, react to the presence of pathogens/danger signals with a large repertoire of functional responses including morphological changes, proliferation, chemotaxis, production/release of cytokines, and phagocytosis. In vitro studies suggest that many of these effector functions are Ca2+-dependent, but our knowledge about in vivo Ca2+ signalling in microglia is rudimentary. This is mostly due to technical reasons, as microglia largely resisted all attempts of in vivo labelling with Ca2+ indicators. Here, we introduce a novel approach, utilizing a microglia-specific microRNA-9-regulated viral vector, enabling the expression of a genetically-encoded ratiometric Ca2+ sensor Twitch-2B in microglia.
Microglia, resident immune cells of the brain, react to the presence of pathogens/danger signals with a large repertoire of functional responses including morphological changes, proliferation, chemotaxis, production/release of cytokines, and phagocytosis. In vitro studies suggest that many of these effector functions are Ca2+-dependent, but our knowledge about in vivo Ca2+ signalling in microglia is rudimentary. This is mostly due to technical reasons, as microglia largely resisted all attempts of in vivo labelling with Ca2+ indicators. Here, we introduce a novel approach, utilizing a microglia-specific microRNA-9-regulated viral vector, enabling the expression of a genetically-encoded ratiometric Ca2+ sensor Twitch-2B in microglia.